14 results
Deciphering stable water isotope records of firn cores from a strongly maritime, high-accumulation site on the Antarctic Peninsula
- Kirstin Hoffmann-Abdi, Hanno Meyer, Francisco Fernandoy, Johannes Freitag, Fyntan M. Shaw, Martin Werner, Elizabeth R. Thomas, Joseph R. McConnell, Christoph Schneider
-
- Journal:
- Journal of Glaciology , First View
- Published online by Cambridge University Press:
- 08 November 2023, pp. 1-19
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Stable water isotope records of six firn cores retrieved from two adjacent plateaus on the northern Antarctic Peninsula between 2014 and 2016 are presented and investigated for their connections with firn-core glacio-chemical data, meteorological records and modelling results. Average annual accumulation rates of 2500 kg m−2 a−1 largely reduce the modification of isotopic signals in the snowpack by post-depositional processes, allowing excellent signal preservation in space and time. Comparison of firn-core and ECHAM6-wiso modelled δ18O and d-excess records reveals a large agreement on annual and sub-annual scales, suggesting firn-core stable water isotopes to be representative of specific synoptic situations. The six firn cores exhibit highly similar isotopic patterns in the overlapping period (2013), which seem to be related to temporal changes in moisture sources rather than local near-surface air temperatures. Backward trajectories calculated with the HYSPLIT model suggest that prominent δ18O minima in 2013 associated with elevated sea salt concentrations are related to long-range moisture transport dominated by westerly winds during positive SAM phases. In contrast, a broad δ18O maximum in the same year accompanied by increased concentrations of black carbon and mineral dust corresponds to the advection of more locally derived moisture with northerly flow components (South America) when the SAM is negative.
Methicillin-resistant Staphylococcus aureus mupirocin resistance rates in a large healthcare system
- Mindy Sampson, Robert Fairman, Elizabeth Palavecino, Werner Bischoff, Julie Williamson, Shelley Keste, Catherine Passaretti
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s85-s86
-
- Article
-
- You have access Access
- Open access
- Export citation
-
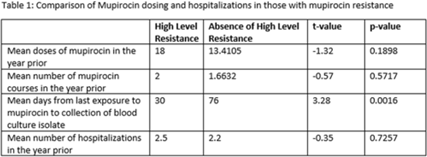
Methicillin-resistant Staphylococcus aureus (MRSA) is a common etiology of hospital-acquired infections (HAIs). One strategy to reduce HAIs due to MRSA involves a multistep decolonization process. This often involves nasal application of mupirocin 2% ointment. In our institution, when individuals meet criteria for decolonization, we recommend 5 days of treatment given twice daily. High levels of mupirocin resistance have been reported in some hospital systems, with >80% of tested isolates being resistant. To better understand our resistance levels, we selected 238 MRSA isolates from blood cultures to be tested for mupirocin resistance to correlate the presence of resistance and use of mupirocin for decolonization. We choose to assess MRSA blood isolates rather than nasal swabs given that we aim to prevent invasive MRSA infections, including blood stream infections, with decolonization. The blood cultures were collected from 11 acute-care facilities within our system from March 2021 through June 2022. High-level resistance was defined as an MIC >1,024 μg/mL according to Clinical and Laboratory Standards Institute guidelines. Of those, 7.14% showed high level resistance, and 76.47% occurred in those who were exposed to mupirocin and 23.53% occurred in those without mupirocin exposure (P = .0094). On average, those with high-level resistance had had more recent exposure to mupirocin compared to those without resistance, which was statistically significant. Also, those with high resistance, on average, received more doses of mupirocin, although this was not statistically significant. Conclusions: More recent and higher number of doses of mupirocin were associated with the development of resistance, which is consistent with what we know from pharmacodynamics of antibiotic resistance with other agents. These findings may be particularly important for those patients who have frequent hospitalizations and often require decolonization. Understanding baseline mupirocin resistance levels in an institution can assist with determining decolonization strategies.
Disclosures: None
The sub-Antarctic islands are increasingly warming in the 21st century
- Werner Nel, David W. Hedding, Elizabeth M. Rudolph
-
- Journal:
- Antarctic Science / Volume 35 / Issue 2 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, pp. 124-126
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
A spatial model of Marion Island's palaeo-ice extent
- Elizabeth M. Rudolph, David W. Hedding, Werner Nel
-
- Journal:
- Antarctic Science / Volume 34 / Issue 5 / October 2022
- Published online by Cambridge University Press:
- 03 August 2022, pp. 365-373
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Sub-Antarctic Marion Island's glacial history has acted as a control on abiotic terrestrial processes and the colonization and distribution of biotic species found on the island today. Recent chronological studies have shown an early deglaciation of the island and identified new geomorphological features associated with past ice dynamics. These permit a reassessment of ice extent during and after the island's last local glacial maximum. In this paper, we provide a revised reconstruction of the island's palaeo-ice extent by using a geomorphology-based approach to delineate palaeo-ice margins and demarcate possible glacial basins. The model presented here provides the needed spatial context for future studies on the variations in the distribution of species (e.g. microorganisms and plant species) and abiotic processes and forms (e.g. soil development and periglacial landforms). In addition, it highlights areas that require improved geophysical assessment in order to produce a more complete island-scale reconstruction of former ice extents (e.g. the west coast).
Associations between childhood maltreatment, poor sleep, and prenatal distress in pregnant adolescents
- Sophie Foss, Hanna C. Gustafsson, Obianuju O. Berry, Alison E. Hipwell, Elizabeth A. Werner, Bradley S. Peterson, Catherine Monk
-
- Journal:
- Development and Psychopathology / Volume 34 / Issue 3 / August 2022
- Published online by Cambridge University Press:
- 08 February 2021, pp. 764-773
-
- Article
- Export citation
-
Childhood maltreatment (CM) is a known risk factor for adolescent pregnancy. Sleep disturbances and psychological distress, both common negative sequelae of CM, often co-occur during pregnancy, although directionality remains unclear. Furthermore, little is known about how CM affects sleep–distress associations during pregnancy. In pregnant adolescents, we examined: (a) whether there are significant predictive associations from CM to sleep quality and distress and (b) bidirectional influences of distress and sleep quality. Healthy pregnant adolescents (n = 204) were recruited before or during the 2nd trimester. CM was assessed at enrollment; sleep quality and distress were assessed in the 2nd and 3rd trimesters. Hypotheses were tested using path analysis. Findings revealed that CM was associated with worse 2nd trimester sleep quality and distress (β = .19, p < .05 for sleep; β = .30, p < .001 for distress). Higher levels of 2nd trimester distress were associated with lower 3rd trimester sleep quality (β = .19, p < .05). Findings provide novel information about (a) associations from CM to prenatal mood and sleep in pregnant adolescents, and (b) sleep–distress directionality over the course of pregnancy. These results have implications for better understanding the ways in which CM potentially exerts influences later in life, and for targeting interventions to address physical and mental health during pregnancy.
Coronavirus disease 2019 (COVID-19) research agenda for healthcare epidemiology
- Part of
- Lona Mody, Ibukunoluwa C. Akinboyo, Hilary M. Babcock, Werner E. Bischoff, Vincent Chi-Chung Cheng, Kathleen Chiotos, Kimberly C. Claeys, K. C. Coffey, Daniel J. Diekema, Curtis J. Donskey, Katherine D. Ellingson, Heather M. Gilmartin, Shruti K. Gohil, Anthony D. Harris, Sara C. Keller, Eili Y. Klein, Sarah L. Krein, Jennie H Kwon, Adam S. Lauring, Daniel J. Livorsi, Eric T. Lofgren, Katreena Merrill, Aaron M. Milstone, Elizabeth A. Monsees, Daniel J. Morgan, Luci P. Perri, Christopher D. Pfeiffer, Clare Rock, Sanjay Saint, Emily Sickbert-Bennett, Felicia Skelton, Katie J. Suda, Thomas R. Talbot, Valerie M. Vaughn, David J. Weber, Timothy L. Wiemken, Mohamed H. Yassin, Matthew J. Ziegler, Deverick J. Anderson
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 2 / February 2022
- Published online by Cambridge University Press:
- 25 January 2021, pp. 156-166
- Print publication:
- February 2022
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This SHEA white paper identifies knowledge gaps and challenges in healthcare epidemiology research related to coronavirus disease 2019 (COVID-19) with a focus on core principles of healthcare epidemiology. These gaps, revealed during the worst phases of the COVID-19 pandemic, are described in 10 sections: epidemiology, outbreak investigation, surveillance, isolation precaution practices, personal protective equipment (PPE), environmental contamination and disinfection, drug and supply shortages, antimicrobial stewardship, healthcare personnel (HCP) occupational safety, and return to work policies. Each section highlights three critical healthcare epidemiology research questions with detailed description provided in supplementary materials. This research agenda calls for translational studies from laboratory-based basic science research to well-designed, large-scale studies and health outcomes research. Research gaps and challenges related to nursing homes and social disparities are included. Collaborations across various disciplines, expertise and across diverse geographic locations will be critical.
8 - Carbon Dioxide Emissions from Subaerial Volcanic Regions
- Edited by Beth N. Orcutt, Isabelle Daniel, Université Claude-Bernard Lyon I, Rajdeep Dasgupta, Rice University, Houston
-
- Book:
- Deep Carbon
- Published online:
- 03 October 2019
- Print publication:
- 17 October 2019, pp 188-236
-
- Chapter
-
- You have access Access
- Open access
- HTML
- Export citation
-
Summary
Recent studies of subaerial volcano carbon flux have challenged previous assumptions about carbon recycling in the mantle and the ratio of ingassing to outgassing. This chapter reviews the current state of knowledge of the flux of carbon from subaerial volcanoes at subduction zones and intraplate locations, as well as through diffuse degassing away from volcanic vents. It also reviews the importance of crustal carbonate assimilation and carbonate platforms on these fluxes. The chapter presents an overview of how these fluxes are estimated – including descriptions of new technologies and recent field campaigns – and the timescales of flux measurements. It also summarizes what is currently known about the flux of carbon versus other volatile elements in these various settings.
Maternal abuse history and reduced fetal heart rate variability: Abuse-related sleep disturbance is a mediator
- Hanna Gustafsson, Colleen Doyle, Michelle Gilchrist, Elizabeth Werner, Catherine Monk
-
- Journal:
- Development and Psychopathology / Volume 29 / Issue 3 / August 2017
- Published online by Cambridge University Press:
- 20 October 2016, pp. 1023-1034
-
- Article
- Export citation
-
The consequences of childhood maltreatment are profound and long lasting. Not only does the victim of abuse suffer as a child, but there is mounting evidence that a history of maltreatment places the next generation at risk for significant psychopathology. Research identifies postnatal factors as affecting this intergenerational transmission of trauma. However, emerging evidence suggests that part of this risk may be transmitted before birth, passed on via abuse-related alterations in the in utero environment that are as yet largely unidentified. To date, no study has directly assessed the influence of pregnant women's abuse history on fetal neurobehavioral development, nor considered trauma-associated poor sleep quality as a mediator reflecting established physiological dysregulation. Using data from 262 pregnant adolescents (ages 14–19), a population at elevated risk for childhood maltreatment, the current study examined maternal emotional abuse history and sleep quality in relation to third-trimester fetal resting heart rate variability, an index of parasympathetic nervous system functioning. The results indicate that maternal emotional abuse history is indirectly associated with lower fetal heart rate variability via abuse-related sleep disturbances. These data demonstrate an association between maternal abuse histories and fetal development, showing that at least part of the intergenerational transmission of risk occurs during pregnancy.
Introduction to the Guideline, and General Principles of Acute Migraine Management
- Irene Worthington, Tamara Pringsheim, Marek J. Gawel, Jonathan Gladstone, Paul Cooper, Esma Dilli, Michel Aube, Elizabeth Leroux, Werner J. Becker, on behalf of the Canadian Headache Society Acute Migraine Treatment Guideline Development Group
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 40 / Issue S3 / September 2013
- Published online by Cambridge University Press:
- 01 July 2015, pp. S4-S9
-
- Article
-
- You have access Access
- Export citation
-
Objectives:
To provide an overview of the objectives and target population of the guideline, and to review the general principles of acute pharmacological migraine therapy.
Methods:A general literature review and several consensus groups were used to formulate an expert consensus for the general use of acute migraine medications.
Results:The objective of the guideline is to assist the physician in choosing an appropriate acute migraine medication for an individual with migraine, and thereby to reduce migraine-related disability. The target population includes adults with episodic migraine (patients with migraine headache < 15 days/month). This guideline is intended primarily for physicians who treat patients with migraine. Other health professionals may also find this guideline helpful. Acute migraine therapy should be considered for the great majority of patients with migraine. A specific acute medication is chosen based on evidence for efficacy, tolerability, migraine attack severity, patient preference, and on the presence of co-existing disorders. General principles of acute migraine therapy include that the response of a patient to any given medication cannot be predicted with certainty, and that treatment early in the attack is generally more effective than treatment later once the migraine attack is fully developed. A suitable treatment approach (stratified or stepped approaches) and drug formulation (injection, tablet, wafer, powdered formulation, or nasal spray) should be chosen based on patient clinical features. Excessively frequent use of acute medications (medication overuse) should be avoided. Two or more acute medications can be combined if necessary.
Conclusions:This guideline provides evidence-based advice on the use of acute medications for migraine, and should provide useful guidance for acute migraine therapy to both health professionals and patients.
Targeted Review: Medications for Acute Migraine Treatment
- Irene Worthington, Tamara Pringsheim, Marek J. Gawel, Jonathan Gladstone, Paul Cooper, Esma Dilli, Michel Aube, Elizabeth Leroux, Werner J. Becker, on behalf of the Canadian Headache Society Acute Migraine Treatment Guideline Development Group
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 40 / Issue S3 / September 2013
- Published online by Cambridge University Press:
- 01 July 2015, pp. S10-S32
-
- Article
-
- You have access Access
- Export citation
-
Objective:
To assess the evidence base for drugs used for acute treatment of episodic migraine (headache on < 14 days a month) in Canada.
Methods:A detailed search strategy was employed to find relevant published clinical trials of drugs used in Canada for the acute treatment of migraine in adults. Primarily meta-analyses and systematic reviews were included. Where these were not available for a drug or were out of date, individual clinical trial reports were utilized. Only double-blind randomized clinical trials with placebo or active drug controls were included in the analysis. Recommendations and levels of evidence were graded according to the principles of the Grading of Recommendations Assessment, Development and Evaluation (GRADE) Working Group, using a consensus group.
Results:Eighteen acute migraine medications and two adjunctive medications were evaluated. Twelve acute medications received a strong recommendation with supporting high quality evidence for use in acute migraine therapy (almotriptan, eletriptan, frovatriptan, naratriptan, rizatriptan, sumatriptan, zolmitriptan, ASA, ibuprofen, naproxen sodium, diclofenac potassium, and acetaminophen). Four acute medications received a weak recommendation for use with low or moderate quality evidence (dihydroergotamine, ergotamine, codeine-containing combination analgesics, and tramadol-containing combination analgesics). Three of these medications were NOT recommended for routine use (ergotamine, and codeine- and tramadol-containing medications), and strong recommendations were made to avoid use of butorphanol and butalbital-containing medications. Both metoclopramide and domperidone received a strong recommendation for use with acute migraine attack medications where necessary.
Conclusion:Our targeted review formulated recommendations for the available acute medications for migraine treatment according to the GRADE method. This should be helpful for practitioners who prescribe medications for acute migraine treatment.
Canadian Headache Society Guideline: Acute Drug Therapy for Migraine Headache
- Irene Worthington, Tamara Pringsheim, Marek J. Gawel, Jonathan Gladstone, Paul Cooper, Esma Dilli, Michel Aube, Elizabeth Leroux, Werner J. Becker, on behalf of the Canadian Headache Society Acute Migraine Treatment Guideline Development Group
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 40 / Issue S3 / September 2013
- Published online by Cambridge University Press:
- 01 July 2015, pp. S1-S3
-
- Article
-
- You have access Access
- Export citation
-
Objectives:
The primary objective of this guideline is to assist the practitioner in choosing an appropriate acute medication for an individual with migraine, based on current evidence in the medical literature and expert consensus. It is focused on patients with episodic migraine (headache on < 14 days a month).
Methods:A detailed search strategy was used to find relevant meta-analyses, systematic reviews and randomized double-blind controlled trials. Recommendations were graded with the Grading of Recommendations Assessment, Development and Evaluation (GRADE) Working Group, using a consensus group. In addition, a general literature review and expert consensus were used for aspects of acute therapy for which randomized controlled trials are not available.
Results:Twelve acute medications received a strong recommendation for use in acute migraine therapy (almotriptan, eletriptan, frovatriptan, naratriptan, rizatriptan, sumatriptan, zolmitriptan, ASA, ibuprofen, naproxen sodium, diclofenac potassium, and acetaminophen). Four received a weak recommendation for use (dihydroergotamine, ergotamine, codeine-containing combination analgesics, and tramadol-containing combination analgesics). Three of these were NOT recommended for routine use (ergotamine, and codeine- and tramadol-containing medications). Strong recommendations were made to avoid use of butorphanol and butalbital-containing medications. Metoclopramide and domperidone were strongly recommended for use where necessary. Our analysis also resulted in the formulation of eight general acute migraine treatment strategies. These were grouped into: 1) two mild-moderate attack strategies, 2) two moderate-severe attack or NSAID failure strategies, 3) three refractory migraine strategies, and 4) a vasoconstrictor unresponsive-contraindicated strategy. Additional strategies were developed for menstrual migraine, migraine during pregnancy, and migraine during lactation.
Conclusion:This guideline provides evidence-based advice on acute pharmacological migraine therapy, and should be helpful to both health professionals and patients. The available medications have been organized into a series of strategies based on patient clinical features. These strategies may help practitioners make appropriate acute medication choices for patients with migraine.
Pharmacological Acute Migraine Treatment Strategies: Choosing the Right Drug for a Specific Patient
- Irene Worthington, Tamara Pringsheim, Marek J. Gawel, Jonathan Gladstone, Paul Cooper, Esma Dilli, Michel Aube, Elizabeth Leroux, Werner J. Becker, on behalf of the Canadian Headache Society Acute Migraine Treatment Guideline Development Group
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 40 / Issue S3 / September 2013
- Published online by Cambridge University Press:
- 01 July 2015, pp. S33-S62
-
- Article
-
- You have access Access
- Export citation
-
Background:
In our targeted review (Section 2), 12 acute medications received a strong recommendation for use in acute migraine therapy while four received a weak recommendation for use. Strong recommendations were made to avoid use of two other medications, except for exceptional circumstances. Two anti-emetics received strong recommendations for use as needed.
Objective:To organize the available acute migraine medications into acute migraine treatment strategies in order to assist the practitioner in choosing a specific medication(s) for an individual patient.
Methods:Acute migraine treatment strategies were developed based on the targeted literature review used for the development of this guideline (Section 2), and a general literature review. Expert consensus groups were used to refine and validate these strategies.
Results:Based on evidence for drug efficacy, drug side effects, migraine severity, and coexistent medical disorders, our analysis resulted in the formulation of eight general acute migraine treatment strategies. These could be grouped into four categories: 1) two mild-moderate attack strategies, 2) two moderate-severe attack or NSAID failure strategies, 3) three refractory migraine strategies, and 4) a vasoconstrictor unresponsive-contraindicated strategy. In addition, strategies were developed for menstrual migraine, migraine during pregnancy, and migraine during lactation. The eight general treatment strategies were coordinated with a “combined acute medication approach” to therapy which used features of both the “stratified” and the “step care across attacks” approaches to acute migraine management.
Conclusions:The available medications for acute migraine treatment can be organized into a series of strategies based on patient clinical features. These strategies may help practitioners make appropriate acute medication choices for patients with migraine.
Contributors
-
- By Cecil S. Ash, Paul Barach, Ulrike Buehner, M. Ross Bullock, Leonardo Canale, Henry G. Chou, Jeffrey A. Claridge, John J. Como, Armagan Dagal, Martin Dauber, James S. Davis, Shalini Dhir, François Donati, Roman Dudaryk, Richard P. Dutton, Talmage D. Egan, Yashar Eshraghi, John R. Fisgus, Jeff Gadsden, Sugantha Ganapathy, Mark A. Gerhardt, Inderjit Gill, Joseph F. Golob, Glenn P. Gravlee, Marcello Guglielmi, Jana Hambley, Peter Hebbard, Elena J. Holak, Khadil Hosein, Ken Johnson, Matthew A. Joy, George W. Kanellakos, Olga Kaslow, Arthur M. Lam, Vanetta Levesque, Jessica Anne Lovich-Sapola, M. Jocelyn Loy, Peter F. Mahoney, Donn Marciniak, Maureen McCunn, Craig C. McFarland, Maroun J. Mhanna, Timothy Moore, Cynthia Nguyen, Maxim Novikov, E. Orestes O’Brien, Ketan P. Parekh, Claire L. Park, Michael J. A. Parr, Elie Rizkala, Steven Roth, Alistair Royse, Colin Royse, Kasia Petelenz Rubin, David Ryan, Claire Sandstrom, Carl I. Schulman, Rishad Shaikh, Ranjita Sharma, Jeffrey H. Silverstein, Peter Slinger, Charles E. Smith, Christopher Smith, Paul Soeding, Rakesh V. Sondekoppam, P. David Soran, Eldar Søreide, Elizabeth A. Steele, Kristian Strand, Dennis M. Super, Kutaiba Tabbaa, Nicholas T. Tarmey, Joshua M. Tobin, Kalpana Tyagaraj, Heather A. Vallier, Sandra Werner, Earl Willis Weyers, William C. Wilson, Shoji Yokobori, Charles J. Yowler
- Edited by Charles E. Smith
-
- Book:
- Trauma Anesthesia
- Published online:
- 05 April 2015
- Print publication:
- 09 April 2015, pp vii-x
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation




